Présentation
Hidradenitis Suppurativa (HS), also known as Verneuil’s disease and acne inversa, is an incurable skin disease manifesting as recurrent, invalidating abscesses. In addition to causing intense pain, HS is commonly associated with disability, depression and anxiety. The estimated worldwide prevalence of HS is 1%, with highest rates in Europe (1-4%) and a >2-fold higher incidence in women. The etiology of HS is unknown. Mutations in gamma-secretase genes were detected in a small subset of HS patients, but their link with the pathophysiology of HS has remained unclear. The sustained production of inflammatory cytokines in skin lesions suggests that HS development involves immune dysregulation. In addition, metagenomic analyses identified a distinctive anaerobic microbiota in HS skin, the expansion of which correlates with lesion severity. In the absence of curative treatments and without mouse models for studying the causes of HS, immunomodulatory drugs and/or antibiotics are prescribed to reduce the disease’s symptoms.
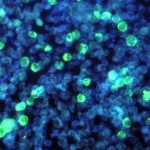
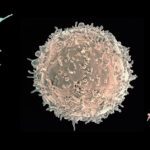
To better understand the origin and interplay between uncontrolled inflammation and cutaneous dysbiosis in HS, we recently conducted an integrated metabolomic and transcriptomic analysis of patient skin. We identified an abnormal induction of the kynurenine pathway (KP) of tryptophan (Trp) catabolism, which correlated with the local release of KP-inducing cytokines. Notably, over-activation of the KP in lesional skin was associated with local and systemic depletion in Trp. Since this essential amino acid is a major energy source for commensal bacteria, we hypothesized that their Trp metabolism may be altered. This was all the more relevant as bacterial degradation of Trp at mucosal surfaces generates indole derivatives regulating tissue inflammation via activation of the Aryl Hydrocarbon Receptor (AHR) transcription factor. In HS skin lesions, we detected a defective activation of AHR coinciding with decreased incidence of AHR ligand-producing bacteria in the resident flora, and locally impaired production of AHR agonists. Our findings thus suggest that HS may be a disease of metabolic imbalance at the host-microbiota interface, a hypothesis that we are currently testing via animal and clinical studies.