Link to Pubmed [PMID] – 37008933
Link to DOI – 10.3389/fendo.2023.1112834
Front Endocrinol (Lausanne) 2023 ; 14(): 1112834
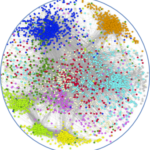
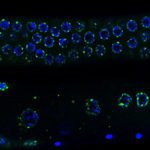
Suitable cryopreservation procedures of pre-pubertal testicular tissue associated with efficient culture conditions are crucial in the fields of fertility preservation and restoration. In vitro spermatogenesis remains a challenging technical procedure to undergo a complete spermatogenesis.The number of haploid cells and more specifically the spermatic yield produced in vitro in mice is still extremely low compared to age-matched in vivo controls and this procedure has never yet been successfully transferred to humans.To evaluate the impact of in vitro culture and freezing procedure, pre-pubertal testicular mice testes were directly cultured until day 4 (D4), D16 and D30 or cryopreserved by controlled slow freezing then cultured until D30. Testes composed of a panel of 6.5 dpp (days postpartum), 10.5 dpp, 22.5 dpp, and 36.5 dpp mice were used as in vivo controls. Testicular tissues were assessed by histological (HES) and immunofluorescence (stimulated by retinoic acid gene 8, STRA8) analyses. Moreover, a detailed transcriptome evaluation study has been carried out to study the gene expression patterns throughout the first in vitro spermatogenic wave.Transcriptomic analyses reveal that cultured tissues expression profiles are almost comparable between D16 and D30; highlighting an abnormal kinetic throughout the second half of the first spermatogenesis during in vitro cultures. In addition, testicular explants have shown dysregulation of their transcriptomic profile compared to controls with genes related to inflammation response, insulin-like growth factor and genes involved in steroidogenesis.The present work first shows that cryopreservation had very little impact on gene expression in testicular tissue, either directly after thawing or after 30 days in culture. Transcriptomic analysis of testis tissue samples is highly informative due to the large number of expressed genes and identified isoforms. This study provides a very valuable basis for future studies concerning in vitro spermatogenesis in mice.