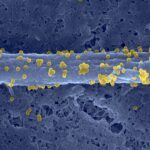
Présentation
Infections remain a major cause of mortality in humans. New infections are emerging, and resistance to antimicrobial drugs is widespread and expanding. There is thus an urgent need to develop novel therapeutic strategies based on rationally-designed drugs blocking the pathogenic effects of microbes on the host. A prerequisite for this is a complete understanding of the pathophysiology of infectious diseases. Systemic infections result from the invasion of hosts by a microbial pathogens, and a critical pathogenic determinant is thus microbial translocation from the external environment into the host and dissemination to protected tissues such as the central nervous system and the fetus. Our project is focused on understanding the molecular mechanisms underlying the ability of certain microbes to cross the intestinal barrier, the blood-brain barrier and/or the placental barrier.
We pursue the following objectives:
- understand how invasive pathogens adhere to host barriers,
- understand how invasive pathogens cross cell monolayer barriers,
- determine microbial fate and dynamics within the host,
- determine how host responses influence barrier vulnerability to invasive pathogens.
Because we address these biological questions in a tissue and whole-host context, this project integrates in vitro, ex vivo, and in vivo approaches. It allows us to address questions in a novel dimension, defining a transition from cellular microbiology to tissular microbiology. Completion of our objectives will provide critical information on key pathophysiological steps critical for the understanding of microbial pathogenesis, and will also improve our basic knowledge of host barriers biology during homeostasis and upon microbial aggression.